Creating a detailed therapy treatment plan is essential for delivering successful mental health care. A well-structured plan acts as a roadmap, guiding clients and therapists toward measurable progress and clear therapeutic goals. In this comprehensive guide, we’ll cover why treatment plans are critical, what elements to include, provide examples and templates, and explain how tools like vcita can simplify your practice.
Why therapy treatment plans are crucial
Therapy treatment plans aren’t just formalities, they’re foundational tools for meaningful progress. These structured outlines help therapists remain focused and organized, ensuring that therapy aligns precisely with each client’s unique needs and objectives. Clients benefit too, gaining clarity, direction, and reassurance about their therapeutic journey.
A robust treatment plan helps:
- Clearly define treatment goals
- Align therapeutic interventions
- Monitor and document progress
- Adjust methods based on effectiveness
- Enhance client engagement and motivation
Components of an effective therapy treatment plan
1. Comprehensive client information
Begin with detailed client background information. This foundational step ensures personalized care and informed interventions:
- Client’s basic contact and emergency details
- Medical and mental health history
- Details about previous treatments and their outcomes
- Diagnostic information and current assessment results
- Information about relevant traumas or significant life events
Example:
“Jane Doe, 34, diagnosed with Generalized Anxiety Disorder. Previous cognitive behavioral therapy sessions showed moderate progress. History includes childhood trauma and recent job loss affecting anxiety levels.”
2. SMART therapeutic goals
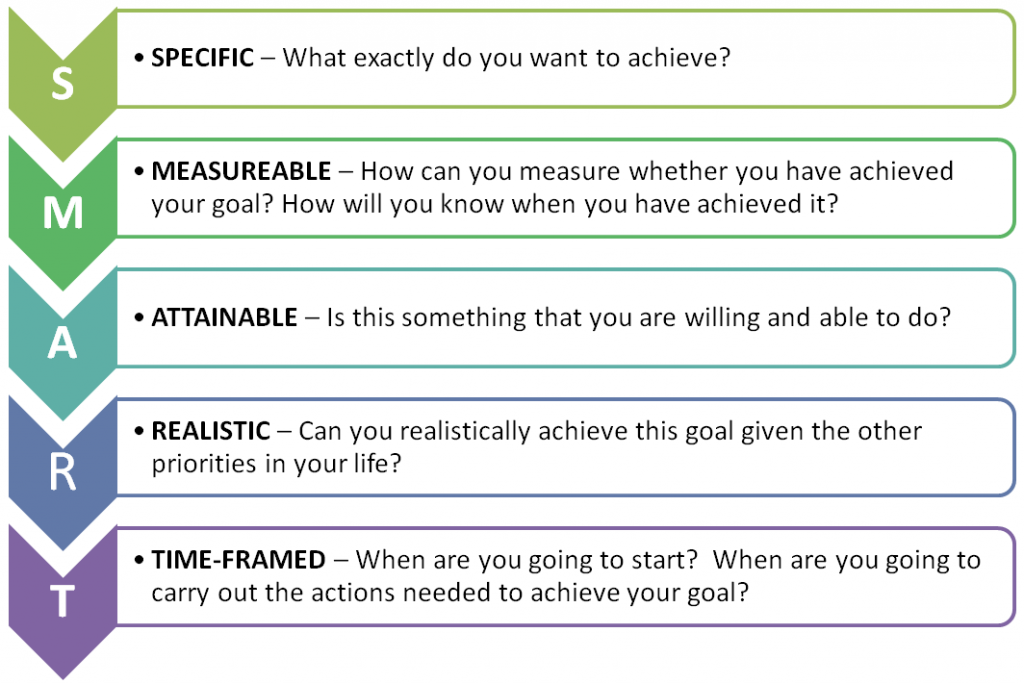
Effective goals are SMART: Specific, Measurable, Attainable, Relevant, and Time-bound. Clearly defined goals promote focused therapy sessions and enhance motivation through visible progress.
Examples:
Specific: “Reduce daily panic attacks from 3 per day to 1 per day.”
Measurable: “Track frequency of panic attacks daily in a journal.”
Attainable: “Utilize daily mindfulness exercises for anxiety management.”
Relevant: “Improvement will help the client re-engage socially and professionally.”
Time-bound: “Achieve reduced frequency within eight weeks.”
SMART goal template:
“Client will [achieve specific outcome] by [taking measurable action] within [time frame], to help [relevance to client’s life or situation].”
Example filled in:
“John will practice 10 minutes of guided mindfulness meditation daily, reducing anxiety symptoms by 50% within six weeks to improve concentration at work.”
3. Treatment methods and interventions
Clearly outline therapeutic methods tailored to the client’s needs:
- Cognitive Behavioral Therapy (CBT)
- Dialectical Behavioral Therapy (DBT)
- Exposure therapy
- Solution-focused brief therapy (SFBT)
- Motivational interviewing
Example:
“Employ CBT techniques such as cognitive restructuring and exposure therapy sessions twice weekly to address social anxiety symptoms.”
4. Progress Monitoring and Adjustment
Regular assessments ensure effectiveness, allowing timely adjustments to treatment strategies:
- Weekly therapy notes
- Regular use of assessment scales (GAD-7 for anxiety, PHQ-9 for depression)
- Client self-report forms
Example:
“Weekly check-ins using GAD-7 indicate decreasing anxiety scores. If no significant change by week 4, introduce additional relaxation strategies.”
Disorder-specific treatment plan examples
Different mental health conditions require tailored approaches. Here are examples for specific disorders:
Anxiety disorder:
Goal: “Client to reduce anxiety attacks from daily to biweekly by week 8.”
Method: “Daily journaling of anxiety triggers and practicing grounding techniques.”
Depression:
Goal: “Increase daily activities from zero to at least three pleasurable activities weekly.”
Method: “Implement behavioral activation strategies and weekly reflection logs.”
Post-traumatic stress disorder (PTSD):
Goal: “Reduce flashback occurrences by 50% within three months.”
Method: “Weekly EMDR sessions and trauma-focused cognitive-behavioral therapy.”
Using templates for efficiency
Therapy treatment plan templates streamline the planning process, ensuring consistency and comprehensive coverage:
Therapy treatment plan template:
Client name:
Diagnosis:
Goal #1:
Objective:
Intervention:
Measurement:
Goal #2:
Objective:
Intervention:
Measurement:
Progress monitoring schedule:
Next review date:
Example:
Client name: Mark T.
Diagnosis: Depression
Goal: Reduce feelings of sadness and hopelessness
Objective: Engage in positive social interactions weekly
Intervention: Schedule and participate in one social event per week
Measurement: Report weekly engagement level in sessions
Progress monitoring schedule: Weekly session evaluations
Next review date: 6 weeks from start date
Enhancing your practice with vcita
vcita simplifies creating and managing treatment plans, allowing therapists to focus more on their clients and less on administration. Key features include:
- Secure Client Management: Maintain comprehensive records safely and accessibly.
- Online Scheduling: Enable clients to conveniently book sessions online, reducing missed appointments.
- Invoicing and Billing: Streamline financial tasks with automated billing and professional invoicing.
- Secure Client Portal: Provide clients easy access to their treatment plans and secure communications with their therapist.
- Efficient Documentation: Use built-in progress notes features for effective tracking of client progress.
Example:
Using vcita, therapist Dr. Elena efficiently schedules and confirms sessions with automated reminders. Her clients securely review session notes and progress reports through the portal, enhancing engagement and transparency. Billing and invoicing are simplified, allowing her more time for direct client interaction.
Key takeaways
- Treatment plans are essential for clarity, direction, and accountability in therapy.
- SMART goals clearly structure therapeutic objectives, enhancing effectiveness.
- Templates save time, ensuring consistent documentation.
- Monitoring progress regularly allows timely adjustments for optimal outcomes.
- Tools like vcita significantly streamline administrative tasks, enhancing therapist-client interactions.
Creating a structured therapy treatment plan enhances client care, promotes accountability, and fosters a successful therapeutic experience. Integrating tools like vcita further simplifies this process, allowing mental health professionals to dedicate their energy fully to client growth and well-being.




























